What is a kidney stone?
The scientific name of kidney stone disease is nephrolithiasis, urolithiasis or renal calculus disease. A kidney stone is a rigid object made from minerals and salt in the urine. Your kidneys filter the blood and eliminate wastes from your body in the urine. When urine concentrates (e.g., when you drink less water), these chemicals crystallise. Gradually they grow and turn into stones. They could be as small as a grain of sand or larger. Rarely do they reach the size of a golf ball.
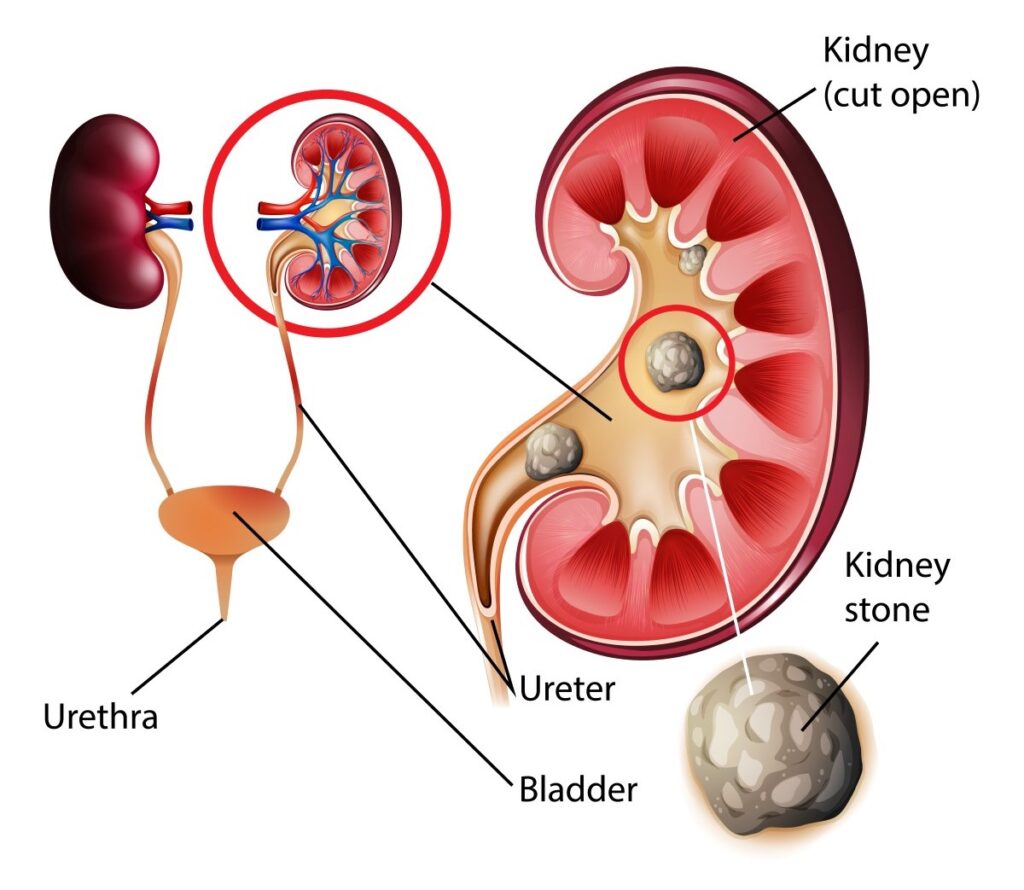
What are kidney stones made of?
There are four main types of kidney stones:
- Calcium stones
80% of kidney stones are calcium stones. There are two types of calcium stones: calcium oxalate and calcium phosphate. Dietary factors, gastric bypass surgeries, and vitamin D supplements increase the risk of calcium oxalate formation. Calcium phosphate stones are more frequent if you have renal tubular acidosis or use certain medications (e.g., topiramate for migraines). - Uric acid stones
This type of stone forms because of acidic urine. Various disorders could make urine more acidic, such as obesity, chronic diarrhoea, type 2 diabetes, gout and a diet with high animal protein. - Struvite stones are a rare type of kidney stone. They form because of chronic urinary tract infections (UTIs).
- Cystine stones are the most rare. They form because of too much cystine in urine (cystinuria). The latter is a metabolic disease which often leads to stone formation in childhood.
Who can have kidney stones?
Anyone can have kidney stones. It’s one of the most prevalent renal diseases. Some factors increase the risk of having a kidney stone. Here is the list of most common dietary rsik factors:
- not drinking enough water
- diet with a low level of calcium
- using calcium and vitamin D supplements
- diet with high levels of animal protein
- diet with high levels of sugars (fructose, sucrose)
- high sodium consumption
- frequent spinach eating
Other non-dietary factors also can increase the risk, e.g.,
- positive family history of kidney stones
- previously having kidney stones
- repeated urinary tract infections
- certain health conditions (obesity, diabetes mellitus, high blood pressure, primary hyperparathyroidism, gout, Crohn’s disease)
- weight loss surgery (e.g., gastric bypass surgery)
- overuse of laxatives, calcium-based antacids, and some medicines for migraine (e.g., topiramate) and depression
How can I know that I have kidney stones?
Kidney stones could be asymptomatic for years. Sometimes, tiny stones travel from the kidney to the ureters, bladder and urethra and pass, without any symptoms. Bigger stones could stay in kidneys or travel and block urine flow, causing severe symptoms. You may have one or more of the following:
- severe, sharp pain in the side and back, below the ribs
- pain that spreads to the lower stomach area and groin
- pain that comes in waves and varies in how intense it feels
- pain or a burning feeling while urinating
- blood in the urine (pink, red or brown urine)
- cloudy or foul-smelling urine
- “gravel” or “sand” in urine (small stones)
- urgent need to urinate
- nausea or vomiting
- fever or chills
The pain caused by a kidney stone is called renal colic. It’s one of the strongest pain sensations known. It may change related to stone movement. For instance, pain could travel from your belly to your lower back or become more intense.
When to see a doctor?
Call your GP if you have any symptoms of kidney stones, such as:
- pain is so severe that you couldn’t find a comfortable position
- pain radiating to the stomach along with vomiting
- pain along with fever and chills
- blood in your urine (haematuria)
- pain when urinating or trouble passing urine
How are kidney stones diagnosed?
Small kidney stones usually cause no symptoms and are often found during a health exam. Your healthcare professional will perform a physical exam and order tests and imaging studies. Diagnosis can also include tests to reveal the chemical structure of the stones.
Blood tests are indicated to diagnose high blood sugar, calcium or uric acid levels.
Urine tests. Your doctor may ask you to collect 24-hour urine to reveal stone-forming substances in your urine.
Imaging scans such as CT scan, ultrasound or X-Ray are often recommended in certain conditions. Also, your healthcare professional may recommend genetic testing if there is a suspicion of primary hyperoxaluria.
How do physicians treat kidney stones?
Treatment of kidney stones depends on stone size, type and location. Small stones that do not obstruct urine flow are treated at home. A healthcare provider may recommend the following:
- drink lots of fluids
- take painkillers or other medications
- urinating through the strainer to catch the stones
If your stone is bigger, you may need inpatient treatment (care in hospital). Treatment options include:
- medicines
- lithotripsy
- percutaneous nephrolithotomy
- ureteroscopy
Can I prevent kidney stones from forming?
After having a kidney stone, later it is more likely. To reduce the risk, your doctor may recommend:
- drinking plenty of water
- eating less salt
- eating plenty of vegetables and fruits
- taking prescribed preventive medications
- Depending on stone type certain foods should be excluded from your diet.
Sources:
UpToDate
American Urological Association
National Kidney Foundation
Mayo Clinic









