What is congenital heart disease?
“Congenital defect” comes from the words congenital, meaning “existing at birth” and “defect”, meaning a problem. The heart is completely formed by the 10th week of pregnancy. If a problem occurs in the way the heart or the blood vessels close to the heart are formed the baby is born with what is called a congenital heart defect, CHD for short. Congenital heart defects are sometimes called congenital heart disease.
Heart defects which keep blood from flowing normally may include:
- A hole in your heart wall.
- Issues with your blood vessels (too many or too few, blood flowing too slowly, to the wrong place or in the wrong direction).
- Problems with your heart valves that control blood flow.
Some cases of CHD are simple and may not cause any symptoms. But others can be life-threatening and require treatment in infancy.
Healthcare providers can detect heart defects early (before or shortly after birth). But sometimes, people don’t get a CHD diagnosis until childhood, adolescence or adulthood.
Heart Anatomy, Function, and Blood Circulation
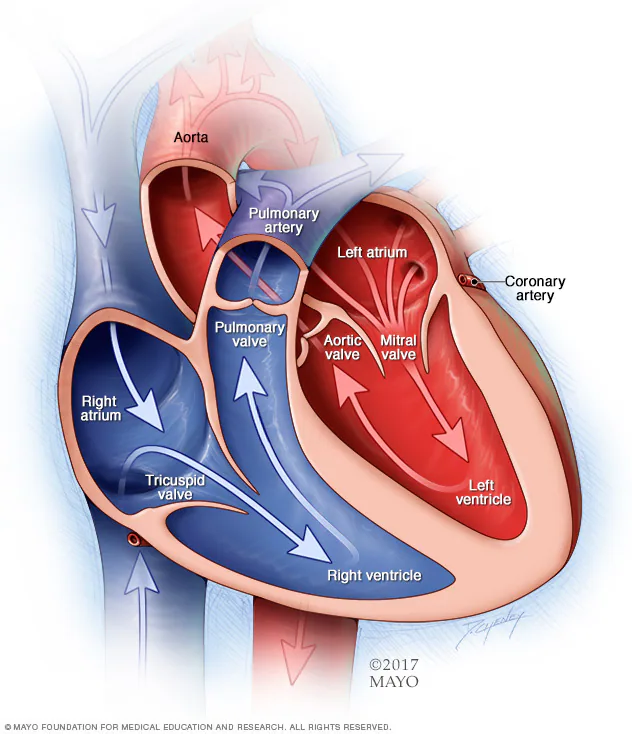
To understand the causes of congenital heart defects, it may help to know how the heart usually works.The typical heart has four chambers. There are two on the right and two on the left.
- The two upper chambers are called the atria.
- The two lower chambers are called the ventricles.
To pump blood through the body, the heart uses its left and right sides for different tasks.
- The right side of the heart moves blood to the lungs through the lung arteries, called the pulmonary arteries.
- In the lungs, the blood gets oxygen. The blood then goes to the heart’s left side through the pulmonary veins.
- The left side of the heart pumps the blood through the body’s main artery, called the aorta. It then goes to the rest of the body.
How common is congenital heart disease?
Congenital heart disease is the most common type of congenital condition. CHDs affect 1% of U.S. births.
What are the types of congenital heart disease?
There are two main groups of CHD:
- Cyanotic (low oxygen in the blood) congenital heart disease.
- Acyanotic (blood oxygen level is acceptable) congenital heart disease.
What is cyanosis?
“Cyan” means blue. Cyanosis is the blueness of the skin, lips, gums, nail beds, and the areas around the eyes and mouth. Many children with CHDs have cyanosis.They are sometimes called “blue babies”.
Healthy children, particularly newborns, may have cyanotic hands and feet when they are cold because their bodies do not deliver enough blood to the tiniest blood vessels, the capillaries.This is called peripheral cyanosis, and is normal. Central cyanosis means that blood throughout the body is not carrying enough oxygen. Children with CHD who have this type of cyanosis may have a blue tinge to the lips, tongue, and nail beds.
Cyanotic congenital heart disease
These heart anomalies reduce the amount of oxygen your heart can deliver to the rest of your body. Babies born with cyanotic congenital heart disease usually have low levels of oxygen and need surgery. Examples include:
- Left heart obstructive lesions: These reduce blood flow between the heart and the rest of your body (systemic blood flow). Examples include hypoplastic left heart syndrome (when your heart is too small on the left side) and interrupted aortic arch (aorta is incomplete).
- Right heart obstructive lesions: These reduce blood flow between your heart and lungs (pulmonary blood flow). Examples include tetralogy of Fallot (a group of four anomalies), Ebstein’s anomaly, pulmonary atresia and tricuspid atresia (valves don’t develop correctly).
- Mixing lesions: The body mixes systemic and pulmonary blood flow. One example is transposition of the great arteries, which means the two main arteries leaving your heart are in the wrong place. Another is truncus arteriosus, when your heart has only one main artery, instead of two, to carry blood to your body.
How might cyanosis affect our child?
Cyanosis by itself is not a problem. However, the way in which your child’s body deals with the low oxygen level is important. The more severe the cyanosis and the longer it continues, the more it will affect your child’s health. Here are the most common effects of cyanosis.
| Effects | Description |
| Growth and Development | Before birth, babies in their mother’s womb have low oxygen levels and grow and develop normally. Babies and children with mild to moderate cyanosis usually have very few effects from cyanosis. Long-term cyanosis interferes with several of the body’s functions. Because the body’s tissues need oxygen to grow and develop normally, very low levels of oxygen can be life threatening. For these reasons, surgery is often done early in the child’s life to reduce or correct the cyanosis. |
| Size | Children with severe cyanosis are often slightly smaller than other children their age. They may not be able to do as much exercise as other children. |
| Activity Level | Muscles, including the heart itself, need a certain level of oxygen to work well. Exercise increases the body’s oxygen requirements. Children will generally limit their own activity level, but you may notice more blueness with exercise, and young babies may get tired out with feeding. |
| Learning | The brain needs enough oxygen to develop and work properly. Some children with cyanosis may take longer to reach their milestones. For example, they may walk and run later than other children the same age. Most children with a CHD do not have significant learning disabilities. |
| Puberty | Studies show that teens with cyanosis reach puberty later than their peers.Your child’s doctor will be watching for this as your child grows, and you can discuss any concerns as they come up. |
| Clubbing | Children with severe cyanosis that lasts for many months or years often develop a condition known as “clubbing”. In clubbing, the ends of the fingers become wide and flat. This different appearance can be very upsetting to some children. Clubbing usually improves after surgery to repair the CHD. |
| Polycythemia | When there is not enough oxygen, the body increases the number of red blood cells fտո carry oxygen. This is called polycythemia and may be associated with bleeding and bruising problems. |
Acyanotic congenital heart disease
This involves an issue that makes blood pump through your body in an abnormal way. For example:
- Hole in the heart: One of your heart’s walls can have an abnormal opening. Depending on the location of the hole, this may be called atrial septal defect, atrioventricular canal, patent ductus arteriosus or ventricular septal defect.
- Problem with the aorta: The aorta is the main artery that carries blood away from your heart to the rest of your body. It can be too narrow (aortic coarctation). Or the aortic valve (which opens and closes to regulate blood flow) may be restricted in opening or have only two flaps instead of three (called bicuspid aortic valve).
- Problem with the pulmonary artery: The pulmonary artery carries blood from the right side of your heart to your lungs to get oxygen. If this artery is too narrow, it’s called pulmonary artery stenosis.
What are the symptoms?
Serious congenital heart defects usually are found soon after birth or during the first few months of life. Symptoms could include:
- Pale gray or blue lips, tongue, or fingernails. Depending on the skin color, these changes may be harder or easier to see.
- Rapid breathing.
- Swelling in the legs, belly or areas around the eyes.
- Shortness of breath during feedings, leading to poor weight gain.
Less-serious congenital heart defects may not be found until later in childhood. Symptoms of congenital heart defects in older children may include:
- Easily getting short of breath during exercise or activity.
- Getting tired very easily during exercise or activity.
- Fainting during exercise or activity.
- Swelling in the hands, ankles or feet.
What causes congenital heart disease?
No one knows what causes most heart defects. You may hear the term “multifactorial causation”.This means that no one thing causes the defect: When certain genetic and environmental factors occur at the same time, a heart defect may result.
Two things that increase the risk of getting a congenital heart defect are the mother’s condition and family history.
Mother’s condition
When a woman is pregnant, what happens to her body can affect the development of her baby’s heart. For example, illnesses such as diabetes (a disease in which the body doesn’t properly produce or use insulin), rubella (German measles), or viral infections can increase the risk of a heart defect.The risk also increases if the mother takes certain prescription or over-the-counter medications (for example, phenytoin, which prevents seizures, Accutane, which is used to treat acne, and lithium salts, which are used to treat certain mental illnesses) or consumes alcohol or “street” drugs.
Family history
If you are the parent of a child with a CHD, the chance of having another baby with some form of CHD increases from about 1% (one in every 100 births) to at least 3% (3 in 100 births). More than one child in a family may have a congenital defect, but this is rare. Medical experts can identify those parents who have a higher risk of having a child born with a CHD, based on the mother’s condition or the parents’ family histories. However, scientists cannot predict which parents will have a child with a CHD because there may be many other reasons besides the mother’s condition and family history.
What are the complications of congenital heart disease?
Congenital heart defects can make you more likely to have:
- Abnormal heart rhythms (arrhythmias).
- Heart failure
- Kidney disease.
- Blood clots.
- Pulmonary hypertension.
- Endocarditis.
- Liver disease.
- Speech issues.
- Attention-deficit/hyperactivity disorder (ADHD).
Complications of congenital heart defects may occur years after the heart condition is treated.
How is congenital heart disease diagnosed?
A congenital heart defect may be diagnosed during pregnancy or after birth. Signs of certain heart defects can be seen on a routine pregnancy ultrasound test (fetal ultrasound).
After a baby is born, a healthcare professional might think there’s a congenital heart defect if the baby has:
- Growth delays.
- Color changes in the lips, tongue or nails.
The healthcare professional may hear a sound, called a murmur, while listening to the child’s heart with a stethoscope. Most heart murmurs are innocent, meaning that there is no heart defect and the murmur isn’t dangerous to your child’s health. However, some murmurs may be caused by blood flow changes to and from the heart.
What tests will be done to diagnose congenital heart disease?
Tests that can help diagnose CHD in newborns, children or adults include:
- Physical exam: During an exam, a healthcare provider will listen to your heart for any abnormal sounds.
- Pulse oximetry. A sensor placed on the fingertip records the amount of oxygen in the blood. Too little oxygen may be a sign of a heart or lung problem.
- Chest X-ray: A chest X-ray takes pictures of the inside of your chest to reveal any structural abnormalities.
- Electrocardiogram: Electrocardiogram (EKG or ECG) measures the electrical activity of your heart.
- Echocardiogram: An echocardiogram (echo) uses ultrasound to create images of your heart’s valves and chambers.
- Heart catheterization: A healthcare provider can tell how well your heart is pumping and circulating blood by performing a heart catheterization. Providers also call it cardiac catheterization or coronary angiography.
- Magnetic resonance imaging (MRI): MRI for heart disease can create detailed pictures of your heart.
How is congenital heart disease treated?
Congenital heart disease treatment may involve:
- A catheter procedure to place a plug into a defect.
- Medications to help your heart work more efficiently or to manage blood pressure.
- A nonsurgical procedure to fix an issue using a closing device.
- Oxygen therapy, which provides higher levels of oxygen than normal room air.
- Prostaglandin E1, which relaxes smooth heart muscle and can keep open the ductus arteriosus (a blood vessel that normally closes after birth), helpս provide needed circulation.
- Surgery to repair an issue, open up blood flow or redirect blood. In severe cases, people need a heart transplant.
Some cases of CHD may not need any treatment. Others are life-threatening and need treatment soon after birth.
How long does it take to recover from this treatment?
Depending on the procedure your child is having, they may need several days, a week or even several months to recover. Ask your child’s provider about recovery for the specific procedure they’re planning.
What can I expect if I have congenital heart disease?
Decades ago, only 10% of children with CHD survived into adulthood. Advances in diagnosis and treatment now help about 90% survive.
Can congenital heart disease be prevented?
There aren’t any proven strategies to prevent CHD. People are born with it, usually from unknown causes. It’s beyond their control.
How can I lower my risk?
You should follow your healthcare provider’s instructions during pregnancy, including:
- Don’t use recreational drugs.
- Get all recommended screening tests during pregnancy to detect problems as early as possible.
- Manage any health conditions, such as diabetes and phenylketonuria.
- Stop smoking and avoid secondhand smoke.
- Avoid alcohol.
When should I go to the emergency room?
Take a person with congenital heart disease to the emergency room or call 911 (or your local emergency service number) if they experience:
- Dizziness.
- Shortness of breath.
- Chest pain.
- Fainting.
Is our child at risk for bacterial endocarditis?
Children with certain CHDs have a higher risk for endocarditis than others. Ask the cardiologist whether your child is at low, moderate or high risk. Children who are at high risk are sometimes given prophylactic antibiotics (medications to prevent the infection).
What is it bacterial endocarditis?
Bacterial endocarditis is an inflammation caused by an infection of the lining of the heart. It starts when bacteria get in the blood and travel through the body. Some of the bacteria attack the lining of the heart in areas where blood flow is not smooth. Bacterial endocarditis is not common, but it is life threatening. Some types of CHDs increase your child’s risk of getting this infection because they cause turbulent blood flow in the heart.
What causes bacterial endocarditis?
The bacteria that cause endocarditis can usually be found in the mouth, digestive tract, and urinary tract. If there is an area that is inflamed, open, bleeding, or there is a dental abscess, the bacteria can move into the blood and travel through the body. Sometimes the bacteria travel to the heart from an infection that’s already in the body such as pneumonia (a lung infection), cellulitis (a skin infection), or a urinary tract infection. Some medical and dental procedures and surgery increase the chance of endocarditis in children at risk.This is because the procedure may cause bleeding, which lets bacteria get into the blood.
How to prevent it?
To help prevent endocarditis, there are two things to remember:
- clean teeth
- antibiotic guidelines for doctors and dentists.
Clean teeth
Make sure that your child has good dental hygiene.This includes regular check-ups with a dentist and regular brushing and flossing of teeth.This helps prevent gum disease, which is a common way for bacteria to get into the blood.
Antibiotic guidelines
There are guidelines for doctors and dentists to follow to help prevent this infection.These guidelines include whether or not to give antibiotics before treatment or surgery that put your child at risk.The American Heart Association’s recommendations have become the standard practice across North America. When you know your child needs antibiotics before medical or dental treatment, discuss this with your family doctor or dentist, who can then order the right medication.
Congenital heart disease in adults
Congenital heart disease (CHD) in adults encompasses a range of heart defects that are present at birth, yet may remain undiagnosed or untreated until later in life. These conditions can vary significantly in severity, potentially impacting the structure and function of the heart.
While many adults with CHD can lead normal, active lives, they may face various complications as they age, including heart failure, arrhythmias, or pulmonary hypertension. Therefore, it is imperative for individuals with CHD to engage in regular follow-up care with a cardiologist who specializes in congenital heart defects. This ongoing management is essential for monitoring their health and addressing any evolving concerns.
Treatment options for adults with CHD are diverse and tailored to the specific defect and accompanying symptoms. These may include pharmacological interventions, lifestyle modifications, and, in some cases, surgical procedures.
Sources:
Mayo Clinic
Cleveland Clinic
Park’s Pediatric Cardiology
UpToDate